Medicare Part C (Medicare Advantage Plans) are provided by private insurance companies to give you more coverage than Original Medicare (Parts A and B) alone. They cover everything in Parts A and B and often include drug coverage and benefits for vision, dental, and hearing care. Medicare Advantage plans and Medicare Supplement plans (Medigap) are often seen as two different ways to address the “gaps” in Original Medicare.
- Medicare Advantage Plans cost anywhere from $0 – $200+ month, with the average premium price at $18/month. Each plan also has its own set of deductibles, copays, coinsurance, and maximum out-of-pocket limits.
- Medicare Advantage Plans are localized, and they have networks of doctors and hospitals that you typically have to stick to to get coverage, unless it’s an emergency. If a doctor or hospital isn’t part of your plan’s network, you often won’t be covered. You may also need referrals or prior authorizations for specialist treatments.
- You must be enrolled in Medicare Parts A and B before enrolling in a Medicare Advantage Plan. You can enroll in a Medicare Advantage Plan during the same Initial Enrollment Period as Parts A and B, during the Open Enrollment Period (Oct 15 – Dec 7), or a few other special periods.
People have all kinds of opinions when it comes to Medicare Advantage Plans.
On one hand, you have advertisements selling Medicare Advantage Plans like they’re the best thing since sliced bread.
On the other, you have Medicare influencers saying they would NEVER choose a Medicare Advantage Plan.
And still, other seniors say they love their Medicare Advantage Plan despite what everyone else tells them.
All of these strong opinions can leave you wondering, “What’s the truth about Medicare Advantage Plans?”
Well… I’m here to demystify this for you.
As the former CEO of Nuvo Health and The Medicare Store, I’ve helped thousands of seniors enroll in the right Medicare plans for them (including Medicare Advantage Plans!).
In this complete Medicare Part C (Advantage Plan) overview, I’ll go over:
- What exactly Medicare Advantage Plans are
- What they cover
- How much they cost
- Part C enrollment periods you need to know about, and
- A comparison between Medicare Advantage Plans and Supplement Plans
Let’s dive in!
What Are Medicare Part C Advantage Plans?
Medicare Advantage Plans are an optional add-on for Original Medicare. They are provided by private insurance companies, and they cover everything in Medicare Part A and Part B and have some extra coverage.
Most Medicare Advantage Plans include drug coverage and benefits for dental, vision, and hearing.
The premiums for Part C are relatively low, with some plans even offering $0 costs. However, most plans have deductibles, copays, and coinsurances that you need to be aware of.
Medicare Advantage Plans also generally have networks. These plans partner up with several local doctors, hospitals, and healthcare facilities to provide low-cost healthcare to their enrollees. However, if you get services outside your plan’s network, you may be subject to higher copays (unless it’s an emergency).
Medicare Advantage Plans may also require referrals and/or prior authorizations before you can get special treatments and procedures. The exact details depend on your provider and plan.
How Does Part C Work?
When you sign up for a Medicare Advantage Plan, Medicare will transfer the responsibility of your healthcare over to your insurance company. They send your insurance company a set amount of money every year, and your insurance company is relatively free to choose how to use that money for your healthcare coverage.
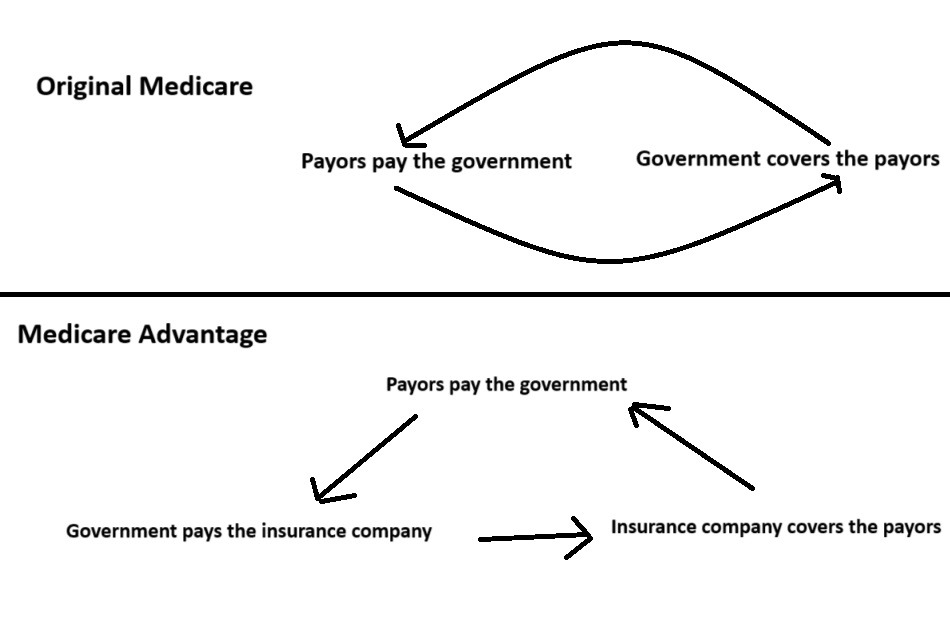
This is why some Medicare Advantage Plans don’t charge you anything to sign up, while others charge relatively low monthly premiums.
When you sign up for a Medicare Advantage Plan, you’re still responsible for paying your Medicare Part B premium.
However, you are usually no longer responsible for the Part A and B deductibles, copays, and coinsurances. Instead, you’ll typically have another payment co-sharing system with your plan provider.
What Do Medicare Part C Advantage Plans Cover?
Medicare Advantage Plans are required to cover everything in Medicare Part A and B, and many plans have drug coverage and benefits of vision, dental, and hearing care.
| Part A (Inpatient) | Part B (Outpatient) |
| Hospital staysSurgeryLab testsSkilled nursing facilitiesHospice careHome health care | Medically necessary servicesPreventive servicesClinical researchAmbulance servicesDurable medical equipmentMental health |
Before signing up for an Medicare Advantage Plan, make sure to check if it also includes a Part D prescription drug plan. Most Medicare Advantage Plans will have one included, but some don’t.
If your Medicare Advantage plan of choice doesn’t have a Part D prescription drug plan included, you need to enroll separately in one to avoid late enrollment penalties.
Finally, Medicare Advantage Plans usually include vision, dental, and hearing care – three things that Original Medicare surprisingly doesn’t cover.
This usually comes in the form of yearly allowances. Although exact coverage for these vary greatly from plan to plan.
How Much Do Medicare Advantage Plans Cost?
Medicare Advantage Plans range from $0/month to $200+/month, but according to the CMS, the average cost in 2024 is $18.50/month. Aside from the premium, you should also take note of your plan’s deductible, copays and coinsurances, and maximum out-of-pocket limit.
- Premiums – The monthly amount you pay to keep your plan. A lot of Medicare Advantage plans have a $0 premium. They can do this because Medicare sends them a fixed amount every year for every person who signs up.
- Deductible – The amount you have to pay out-of-pocket before your coverage starts. Medicare Advantage plans are typically free to set how high their deductibles are.
- Copays – A fixed amount you have to pay for a service. Medicare Advantage plans typically set their copays for each service. Ex: some plans might make you make a $20 copay for every doctor visit.
- Coinsurance – A percentage of the bill you’re responsible for paying. Each plan normally sets its coinsurance rates for services. Ex: some plans make you pay 20% for your outpatient bills.
- Maximum Out-of-Pocket (MOOP) – Once your healthcare out-of-pocket spending for the year reaches the plan’s MOOP, your insurance company will cover 100% of additional bills. This is usually as long as you get services in their network. Plans can set their own MOOP limits.
Because Medicare Advantage Plans aren’t standardized, the exact costs for these vary greatly from provider to provider.
To help you get an idea of how much a Part C plan costs, here are the prices of some top-rated plans from different cities, purely for the sake of example:
Disclaimer: The plans and numbers shown below were taken from Medicare’s plan finder tool for sample purposes. Also, the details below are just some of the numbers of these plans. Always check a plan’s full details before enrolling. To find and compare Medicare Advantage Plans available in your area, you may use Medicare’s tool or contact us for help at +1 877-360-6565 (TTY: 771).
Medicare Advantage Sample Costs in New York City, New York
| Sample Plan #1 (PPO) | Sample Plan #2 (HMO) | Sample Plan #3 (HMO-POS) | |
| Premium: | $0 | $39.20 | $43 |
| Deductible: | Health: $0 Drugs: N/A | Health: $0 Drugs: $545 | Health: $0 Drugs: $350 |
| MOOP: | $8,500 (in-network) $12,500 (out-of-network) | $8,850 | $7,550 |
| Inpatient copays or coinsurance: | In-network:$395/day (day 1-5)$0/day (day 6-90) Out-of-network:50% per stay | $450/day (day 1-5)$0/day (day 6 onwards) | $390/day (day 1-5)$0/day (day 6 onwards) |
| Outpatient copays or coinsurance: | $0 – $500 copay per visit (in-network) 50% coinsurance per visit (out-of-network) | 20% coinsurance | $0 – $390 copay per visit |
| Other Coverage: | ❌ Drugs✅ Vision✅ Dental✅Hearing | ✅ Drugs✅ Vision✅ Dental✅Hearing | ✅ Drugs✅ Vision✅ Dental✅Hearing |
Medicare Advantage Sample Costs in Indianapolis, Indiana
| Sample Plan #1 (HMO) | Sample Plan #2 (PPO) | Sample Plan #3 (Regional PPO) | |
| Premium: | $0 | $27 | $73 |
| Deductible: | Health: $0 Drugs: $0 | Health: $0 Drugs: $0 | Health: $500 Drugs: $0 |
| MOOP: | $3,100 | $3,800 (in-network) $5,750 (in and out-of-network) | $6,400 (in-network) $10,000 (in and out-of-network) |
| Inpatient copays or coinsurance: | $340/day (day 1-6)$0 (day 7-90) | In-network:$370/day (day 1-5)$0 (day 6 onwards) Out-of-network:40% per stay | In-network:$290/day (day 1-7)$0 (day 8-90) Out-of-network:30% per stay |
| Outpatient copays or coinsurance: | $350 per visit | In-network:$0 – $370 copay per visit Out-of-network:$400 copay per visit | In-network:$0 copay or 20% coinsurance per visit Out-of-network:40% coinsurance per visit |
| Other Coverage: | ✅ Drugs✅ Vision✅ Dental✅Hearing | ✅ Drugs✅ Vision✅ Dental✅Hearing | ✅ Drugs✅ Vision✅ Dental❌Hearing |
Medicare Advantage Sample Costs in Fresno, California
| Sample Plan #1 (HMO) | Sample Plan #2 (HMO) | Sample Plan #3 (HMO) | |
| Premium: | $0 | $25 | $70 |
| Deductible: | Health: $0 Drugs: $0 | Health: $0 Drugs: $0 | Health: $0 Drugs: $0 |
| MOOP: | $999 | $3,200 | $2,500 |
| Inpatient copays or coinsurance: | $0 (day 1-3)$50/day (day 4-7)$0 (day 8-90) | $200/day (day 1-5)$0 (day 6 onwards) | $230/day (day 1-5)$0 (day 6 onwards) |
| Outpatient copays or coinsurance: | $85 copay per visit | $0 – $100 copay per visit | $0 – $175 copay per visit |
| Other Coverage: | ✅ Drugs✅ Vision✅ Dental✅Hearing | ✅ Drugs✅ Vision✅ Dental✅Hearing | ✅ Drugs✅ Vision✅ Dental❌Hearing |
What Are the Different Kinds of Advantage Plans?
There are 5 types of Medicare Advantage Plans: HMOs, PPOs, PFFS, SNPs, and MSAs.
- Health Maintenance Organization (HMO) – HMOs are one of the most common types of Medicare Advantage Plans. These plans usually only cover you in their network of doctors and hospitals and require referrals to see a specialist. They also often require you to choose a primary care doctor. Most HMOs have drug coverage, as well as other benefits.
- Preferred Provider Organization (PPO) – PPOs are another common type of Medicare Advantage Plan. Unlike HMOs, PPOs usually allow you to get care outside their network (but with higher cost sharing). They don’t require you to have a primary care doctor or get referrals to see a specialist. Most PPOs also have drug plans and other benefits.
- Private Fee-for-Service (PFFS) – PFFS plans typically don’t have networks of providers. However, normally your healthcare provider must agree to treat you and accept your plan’s payment terms before you can get coverage. Some PFFS plans have network providers that always accept to treat you.
- Special Needs Plan (SNP) – SNPs are generally available for people who have qualifying health conditions like cardiovascular disorders, diabetes, chronic heart failure, etc., or people who are both in Medicare and Medicaid. SNPs are tailored to your specific condition, and they can be either an HMO or PPO.
- Medicare Savings Account (MSA) – MSAs work similarly to Health Savings Accounts (HSAs). They combine high-deductible insurance with a savings account, which they deposit money into every year. MSAs typically don’t have a network, or drug coverage, and don’t require a primary care doctor or referrals.
When Can You Enroll in Medicare Part C?
You can enroll in a Medicare Part C plan as soon as you become eligible for Medicare (7 months around the time you turn 65). There are also enrollment periods every year when you can change plans or opt out of your Medicare Advantage Plan.
The Medicare Advantage Plan enrollment periods you need to know about are the:
- Initial Coverage Election Period (ICEP)
- Open Enrollment Period (OEP)
- Medicare Advantage Open Enrollment Period (MA OEP)
- Special Enrollment Period (SEP)
Initial Coverage Election Period (ICEP)
Your ICEP is the first time you become eligible to enroll in an MA plan. This starts 3 months before your Medicare Part A and B coverage begins, and ends once your Part A and B coverage starts or once your Original Medicare Initial Enrollment Period Ends (whichever is later).
Practically speaking, most people’s ICEP starts at the same time they first become eligible for Medicare (their Initial Enrollment Period or IEP).
This happens when people turn 65. The IEP starts 3 months before your birth month and ends 3 months after it. So if your birthday is July 20, your IEP will run from April 1 to October 31.
However, if you choose to delay enrolling in Medicare Part B for any reason, your ICEP won’t be the same as your Original Medicare IEP.
Instead, it’ll run for 3 months before your Part B coverage begins and will end on the same day your Part B starts.
Confusing?
I know it is. But if you could remember just one thing from above, it’s that if you’re enrolling in an MA for the first time, the best time to do this is 1-3 months before your Part B coverage begins!
Open Enrollment Period (OEP)
The Open Enrollment Period runs from October 15 to December 7 every year. During this period, you can enroll in, switch, or opt out of Medicare Advantage Plans.
Note: the Open Enrollment Period (OEP) is sometimes also called the Annual Election Period (AEP).
If you already have Original Medicare but missed your ICEP, you can enroll in a Medicare Advantage plan during the Open Enrollment Period that happens every year. Your Medicare Advantage Plan will normally take effect on January 1 of the following year.
If you signed up for a Medicare Supplement Plan, but want to switch to a Medicare Advantage Plan instead, you can also do this during the Open Enrollment Period.
Another thing to note is that Medicare Advantage Plans can change their terms every year. If you don’t like your plan’s changes, or you find a better Medicare Advantage plan for you, you can switch during this Open Enrollment Period.
Finally, if you want to switch from a Medicare Advantage plan back to Original Medicare, this is also the time to do it.
Medicare Advantage Open Enrollment Period (MA OEP)
The MA OEP runs from January 1 to March 31 every year. During this period, you can switch to a different Medicare Advantage Plan, or switch from an MA plan back to Original Medicare.
Unlike the Open Enrollment Period, this period is only for people who are already enrolled in a Medicare Advantage Plan. You normally can’t switch from Original Medicare to an MA plan during this time.
Any plan changes made in the MA OEP will normally take effect on the first day of the following month.
Special Enrollment Period (SEP)
If you qualify for a Special Enrollment Period, you can join a Medicare Advantage Plan outside the usual enrollment periods. Some qualifiers include moving to a new location, losing coverage, or your insurance provider stopping your plan.
If you get into one of these situations, you’ll usually have a 3-month period where you can enroll or switch Medicare Advantage Plans.
For a full list of Special Enrollment Periods for MA plans, check Medicare’s website.
Should You Enroll in a Medicare Advantage Plan?
Now for the big question…
Should YOU enroll in a Medicare Advantage plan?
Like all things Medicare, it all depends on your exact situation.
In Medicare circles, it’s generally accepted that getting a Medicare Advantage Plan provides more coverage than staying on Original Medicare only (without even enrolling in a Medicare Supplement Plan).
This is because even though Original Medicare covers around 80% of your healthcare costs, it has no cost caps. If you get a major disease or condition, your out-of-pocket spending could reach $10,000 (or even $100,000)!
Medicare Advantage plans have low premiums, cover everything in Original Medicare, and most also have drug plans, other benefits, and maximum out-of-pocket limits.
The real question comes when you compare Medicare Advantage Plans to your other option: Medicare Supplement Plans.
So let’s take a closer look at that.
All of these numbers are general and shouldn’t be seen as a guarantee of what you’ll find:
Medicare Advantage (Part C) vs Medicare Supplement (Medigap) Plans
| Medicare Advantage Plans | Medicare Supplement Plans | |
| Average Premiums: | Lower $0 – $200+($18 average) | Higher Plan G: $150 – $350 Plan N: $80 – $250 |
| Network: | Most plans have networks of doctors and hospitals | Plans will cover you for any doctor or hospital that accepts Medicare |
| Coverage: | No standardization As long as they cover everything in Medicare Part A and B, Medicare Advantage Plans can usually cover as much as they want | 10 standardized plans (Plan A, B, C, D, F, G, K, L, M, and N) All plans must provide the same coverage regardless of insurance company |
| Referrals and Prior Authorizations: | Usually yes | No |
| Vision, Dental, and Hearing Benefits: | Usually yes | No |
| Drug Coverage: | Usually included | Not included. You’ll sign up for a separate Part D drug plan. |
| Costs: | Typically more out-of-pocket costs Exact costs depend on your plan. Most include: DeductiblesCopaysCoinsurancesMaximum out-of-pocket limits | Typically less out-of-pocket costs Exact costs depend on which plan you choose. Plan G: Part B Deductible only Plan N: Part B Deductible, copays for office and ER visits, Part B excess charges |
| Enrollment: | Can enroll during the ICEP, OEP, or SEP No medical underwriting process | Can enroll at any time. However, if you enroll outside your Initial Enrollment Period (6 months after Part B starts), you may be subject to a medical underwriting process |
In a nutshell, we usually find that:
Medicare Supplement Plans are common for people who have more income and want flexibility and predictable costs. With something like Medigap Plan G, your healthcare costs will only be your premiums for Part B and Plan G, and the Part B deductible (and a Part D plan if you get one).
Medicare Advantage Plans are common for people who want to save money and have a good network of doctors and hospitals in their area. They’re also common for people who want to spend less on vision, dental, and hearing care.
Note: This is a general recommendation. The best plan for YOU will always depend on your exact situation. That’s why it’s best to talk with a broker to find options in your area. If you want professional and unbiased options, call xxx-xxx-xxxx!
Conclusion: 7 Practical Medicare Part C Tips You Need to Know
Before I close this article, I’d like to give you some professional tips when it comes to Medicare Advantage Plans.
- Check The Network.
For the lowest cost on your healthcare services, it’s a good idea to check a plan’s network first to see if there are several doctors and hospitals in your area that accept the plan. This way, you won’t be subject to higher cost-sharing that most Medicare Advantage Plans have when you go outside their network.
- Check The Drug Coverage
If you’re taking prescription medications, you’ll want to sign up for a Medicare Advantage Plan that covers your meds, unless you already have creditable coverage elsewhere. You can do this by checking your plan’s drug formulary.
- Go For a Trusted Carrier
Many companies offer Medicare Advantage Plans, but it’s generally a good idea to stick with a trusted and reputable carrier.
Remember, you’ll need referrals and prior authorizations for some special treatments. So you’ll want a company that has a good track record of responding to these requests.
Medicare’s Plan Finder also has star ratings you may want to check before enrolling.
- Don’t Get Carried Away by Ads
Many sales agents selling Medicare Advantage plans go heavy on advertising. They advertise on TV, radio, telephone, and the internet to try and get people to enroll in their plans.
There’s plenty of over-promising in these ads. Some sales agents even try to “trick” people into signing up for their plans (such as inflating their numbers or posing as Medicare).
This has become such a big problem that Medicare is cracking down on these ads. Nowadays, laws are coming out regulating these ads – but some people are still finding workarounds.
Whatever the case, you should be very careful when it comes to Medicare ads.
As a rule of thumb, avoid signing up for a plan if it comes to you. Instead, you want to be the one to go to the company to get a plan that you already know about.
- Always Review Yearly Changes
Medicare Advantage Plans change their terms every year. That’s why right before the Open Enrollment Period, your Medicare Advantage provider will send you a summary of these changes.
It’s very important to review these changes. If you don’t like them, then you can shop for a better Medicare Advantage Plan.
Even if you are okay with the changes, there may be a new Medicare Advantage Plan in your area that’s significantly better than your current one.
When it comes to Medicare Advantage plans, you may want to avoid renewing for convenience’s sake.
- Talk With a Licensed Insurance Broker
If you’re overwhelmed with the number of plans in your area, an easy way to find a good plan is by talking to a licensed insurance broker.
If you talk directly to an insurance company, they’ll probably only recommend their plans.
On the other hand, independent brokers are contracted with many insurance companies. This way, they can typically be unbiased, and recommend plans for you based on your specific needs.
Professional brokers are also paid by commission by the plan itself, so you don’t have to pay anything for their services.
If you’d like to talk to a professional to find plans in your area, contact +1 877-360-6565 (TTY: 771)! You can get help finding the right plan, or ask any questions you have regarding Medicare.

Calvin Bagley is the founder of PlanFit, The Medicare Store, and Nuvo Health. He and his team have helped over 60,000 people navigate Medicare options, and he’s a nationally recognized speaker in the Medicare industry. Most importantly, he’s someone who believes every American deserves clear, honest information without pressure.

